Liz Wilcox, research projects coordinator at BC Cancer, with sons Nathan (left) and Graham (right)
Before Liz Wilcox became pregnant with her second child, she thought she'd likely have another caesarean birth, also known as a C-section. Her first child, Graham, was delivered via emergency C-section in 2018 after he experienced fetal distress during labour. She often heard from family and friends that it's easier and safer to schedule a repeat C-section as opposed to trying for a vaginal birth after caesarean (VBAC) .
"Even as a health-care researcher, I was really surprised to learn that over 75 per cent of people in B.C. who've had a C-section before are good candidates for VBAC. It's not a statistic I hear a lot when I talk to families or parents who are expecting again."
B.C. has the highest rate of caesarean births in Canada at almost 37 per cent, compared to the national average of 28 per cent. In some areas like the Fraser Health Authority, nearly 42 per cent of babies are delivered via C-section. The province also has very high repeat C-section rates, even though VBAC is considered safer for both mom and baby in low-risk pregnancies.

Misinformation and miscommunication about VBAC drove Dr. Sarah Munro, an affiliate member of
Women's Health Research Institute, and her team to develop an interactive patient decision tool called
My Next Birth . Working in partnership with
Perinatal Services BC , regional health authorities, the BC Ministry of Health, and patient partners, the team aimed to give families information on delivery options when they're in-between pregnancies.
"Families often have to wait until the next pregnancy to start discussing options with their care team," says Dr. Munro. "We really want them to have the information sooner so they can make an informed decision about their next birth. If people don't know their options they'll fall back to what they are already know, and in many cases, this likely means another C-section."
My Next Birth officially launched in May and is available to anyone in B.C., whether they're planning to get pregnant again or only recently delivered a baby. In fact, Dr. Munro says the best time to use the tool is actually within the first six weeks after giving birth.
"This early postpartum period is a key time to review what happened after the C-section. The event is fresh in everyone's mind and your health-care team will have the best information. Once a patient gets discharged from care at the six-week checkup, that opportunity is lost."

The
My Next Birth tool helps people who have previously had a C-section review their options. They'll find questions and information tailored to their specific values and needs. It also factors in where they live geographically in B.C. so they can consider what resources are available locally. After they go through the website, they get a personalized summary printout to guide conversations and questions with their health-care team.
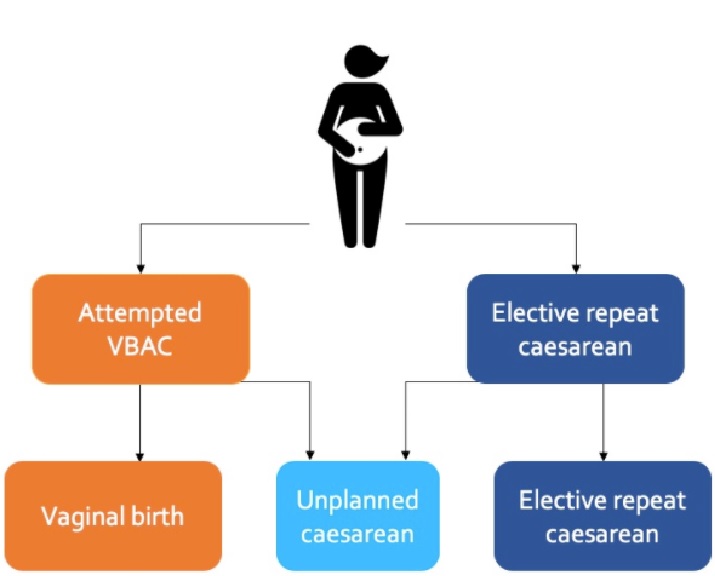
For care providers, the tool includes a decision support algorithm that walks them through the patient's journey and a list of conversation prompts to guide discussions after the C-section — in the early postpartum period, at the six-week postpartum checkup, and then into the next pregnancy.
Liz was already working as a research methodologist with the My Next Birth team when she became pregnant with her second son. That's when she became the perfect tester for the tool.
"It was eye-opening and gave me different questions to consider, like whether I was going to have more children," says Liz. "I felt armed with information when discussing my birth options with my obstetrician. It helped me advocate for a VBAC and prepared me for what my OB might say."
While Liz ultimately delivered baby Nathan via emergency C-section in July 2020 after her labour failed to progress, she's glad she used My Next Birth to explore her options.
"It's important for those expecting again to feel empowered to talk about what they want with their care provider, and what's important to them. I'm hoping this tool will help families be active participants in their care."
